Ontario intensive care units see jump in COVID-19 patients
The number of confirmed COVID-19 patients in intensive care units around Ontario has doubled in less than two days, prompting concern that the virus has actually been spreading more rapidly than previously thought.
There were 43 patients hospitalized in Ontario's ICUs on Friday, up from 29 on Thursday and 17 on Wednesday, according to figures from the province's associate chief medical officer of health, Dr. Barbara Yaffe.
That rapid jump in the number of patients in critical care is distressing, said Dr. David Fisman, a University of Toronto epidemiologist.
The data "suggests that the epidemic three weeks ago was likely much larger than we previously believed," said Fisman. "It also suggests that we may see a rapid surge in ICU occupancy, potentially leading to a situation like that in New York, if this growth continues."
The number of patients in intensive care is considered a crucial measure because ICUs have been the first part of the hospital systems to be overwhelmed in the COVID-19 outbreaks in Italy, Spain and New York. Evidence from the pandemic so far suggests it typically takes two to three weeks for someone to go from contracting the virus to showing symptoms to needing hospitalization.
Fisman said a crucial detail is whether the bulk of the patients in Ontario ICUs contracted COVID-19 in nursing homes or in the community, something the province's ministry of health has not made public.
Calls for 'clear, transparent' information sharing
If the cases in ICU consist largely of people from long-term care homes, that may mean the spread of the coronavirus in the community was not so rapid as the hospitalization data imply.
Fisman is calling for "clear, transparent and honest information sharing" from the Ministry of Health and Public Health Ontario.
Senior provincial health officials are declining to say specifically where those 43 patients are hospitalized.
However, some hospitals have begun publicly reporting their numbers of patients who have tested positive for COVID-19. Based on those public postings and inquiries by CBC News, here are some numbers of patients in ICUs:
6 - Southlake Regional Health Centre in Newmarket
5 - Mackenzie Health in Richmond Hill
3 - London Health Sciences Centre
3 - University Health Network, which includes Toronto General and Toronto Western hospitals
12 - at other Toronto hospitals, according to information made public by Mayor John Tory on Friday
1 - at Brampton Civic Hospital, part of the William Osler Health System
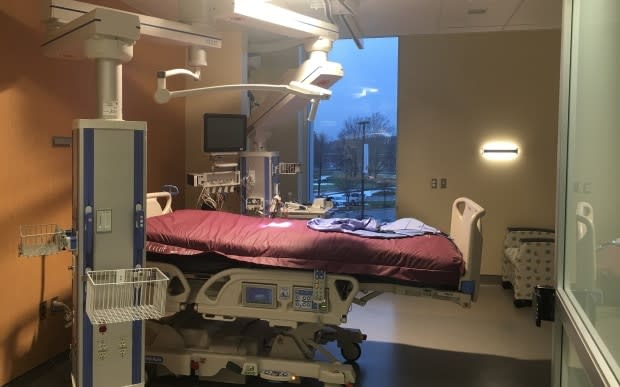
On Friday, Ministry of Health officials gave assurances that the province's hospitals have cleared space in critical care units, in part through postponing non-emergency surgeries, and have plans to ramp up capacity if necessary.
About 68 per cent of ICU beds across the province are currently occupied, leaving about 400 ICU spots available, the officials said during a briefing with reporters.
Testing regime picking up cases 1 or 2 weeks after infection
However the most-specialized ICU beds — known as Level 3, typically what is needed to care for the most severely ill COVID-19 patients — are running at 85 per cent capacity.
An updated model by a group of Toronto-based scientists suggests more than 700 patients in Ontario will need ICU beds by early April, given the current rate of spread of the virus. The epidemiology model was created by a team from the University of Toronto, University Health Network and Sunnybrook Health Sciences Centre.
The next few days will reveal crucial information about Ontario's efforts to slow the spread of the virus, according to numerous health officials.
That's because the province's physical distancing measures began in mid-March, with the announcement of school closures and the ensuing declaration of a state of emergency. Ontario's testing regime is typically picking up cases one to two weeks after contracting the virus.
The evidence of success will be whether the daily increase in new cases starts to slow down.
While provincial officials are preparing for the possibility of a rapid surge in cases, as happened in Italy, the trend in Ontario does not appear that steep, said Dr. Kevin Smith, CEO of the University Health Network, serving as co-chair of the critical care section of the province's COVID-19 response team.
"It could dramatically turn around if our physical distancing isn't consistent and the recently returning Canadians aren't following the segregation rules," said Smith during the Friday briefing. "We won't really know this probably for another three to five days."
Officials and epidemiologists are uncertain when Ontario's COVID-19 caseload will hit its peak or when the demands on hospitals will be the greatest.
"We're basically recalibrating the models pretty much every day based on the data," said Helen Angus, deputy minister of health and chair of the province's COVID-19 command table. "I can't give you a precise date of the peak or the shape of the curve at the moment."

In addition to the six ICU patients at Southlake who have tested positive, three more are presumed to have the virus, the hospital's CEO Arden Krystal said Friday evening.
"I anticipate within a matter of a number of days our main ICU [with 15 beds] will have COVID patients only," said Krystal in an interview with CBC News. "These are very sick patients and they require a lot of resources."
At 500 beds, Southlake is one of the largest hospitals in the province.
"We have many plans in place to continue to expand our ICU capacity and we have significant stock of ventilators," Krystal said. The hospital could move patients who don't have COVID-19 from the main ICU to other critical care wards, such as its cardiac critical care unit.
Southlake officials decided to post their COVID-19 patient numbers publicly to "quell the rumour mill" and to educate the public about the importance of physical distancing in slowing the spread of the virus, said Krystal.
"It makes it more real for the community," she said. "They realize that it's really happening."
Quick facts about Ontario's hospitals
2,053 adult intensive care beds
1,321 of those are equipped with ventilators
209 ventilators in the provincial stockpile are ready to be deployed now
around 600 other ventilators can be made available for hospitals through various means, including Ontario's share of a federal stockpile
800 new ventilators have been ordered by the province; Only 40 have been received so far, and it will likely take months for the bulk to arrive, according to officials
Overall hospital occupancy rate in Ontario is currently at 77 per cent, while last year at this time it was averaging 97 per cent. That means about 6,400 hospital beds are now available.
Source: Ontario Ministry of Health briefing

 Yahoo Movies
Yahoo Movies 