'No clear answer': Few clues in case of girl sickened by foreign bacteria as others test positive
A medical mystery emerging in three states took a concerning turn over the weekend as seven family members in Texas tested positive for potential exposure to a deadly type of bacteria that isn’t supposed to be found in the continental United States.
Disease detectives from the Centers for Disease Control and Prevention have told the family of Lylah Baker, a 4-year-old girl hospitalized in Dallas, that blood tests show several of them have antibodies to the bacteria, called Burkholderia pseudomallei, that has sickened Lylah with devastating consequences.
None of Lylah's family members are currently sick. But Burkholderia pseudomallei bacteria are insidious and have the potential in rare cases to remain dormant in a person’s body for more than 20 years, before reactivating and causing a disease called melioidosis.
“That’s what we’re worried about,” Ashley Kennon, Lylah’s aunt, who is also a nurse, told me Monday as she was headed to get additional blood testing done for the CDC. Kennon said she is among the seven members who have tested positive in this close-knit family that lives in Bells, Texas, a small town about 60 miles northeast of Dallas.
The CDC has said that it suspects the source of the unusual outbreak – which has seriously sickened Lylah and two adults in Minnesota and Kansas, one fatally – could be an imported product or animal that was carrying the bacteria. These bacteria primarily are found in parts of Asia and Australia, and infections generally occur from direct contact with contaminated soil or water.
Too often, disease outbreaks and investigations are chronicled by their numbers. But each of those numbers is a person and a family needing answers.
'Doctors are still stunned': How did foreign bacteria leave a Texas girl with brain damage?

Lylah, who had no preexisting health problems, has suffered brain damage from her infection. The three cases are highly unusual because none of the patients or their families have traveled outside the continental United States. And despite the fact that the patients don’t know one another and live in different states, the CDC’s genomic tests on the bacteria suggest a common source of exposure.
Despite collecting and testing household products and environmental samples from all three patients, top CDC investigator cautioned that the agency might not be able to find the source of the outbreak.
“A number of hypotheses are being evaluated, but there is no clear answer at this time,” said William Bower, the epidemiology team lead for CDC’s Bacterial Special Pathogens Branch. “CDC and state partners are working hard to investigate, but there is a possibility that we will not be able to identify the source of these infections.”
Why solving medical mysteries matters, in cases small and large
This investigation, on a small scale, is an example of how challenging it can be to trace the source of an outbreak – even when everyone is working together and willing to explore all plausible theories.
Magnify this level of difficulty many fold for what it is going to take to find the source of the virus that causes COVID-19, especially given the lack of cooperation by China – the country at the epicenter of the pandemic’s first cases. Last week, the Chinese government said it is refusing to participate in a second phase of a World Health Organization investigation because the investigation would have included scrutiny of any potential role played by laboratory research in Wuhan, in addition to potential wildlife or animal market sources.
'I remember it very well': Dr. Fauci describes a secret meeting to talk about COVID origins
Could an accident have caused COVID-19?: Why the Wuhan lab-leak theory shouldn't be dismissed
Whether it’s millions sickened and killed around the globe from COVID-19 or a little girl in a Dallas hospital having to relearn how to talk and walk and swallow because of a rare bacteria, these disease investigations aren’t supposed to be about politics or countries or pride or blame. They are about real people – those who have paid a terrible price from disease and those who can be spared by scientists following the evidence.
Lylah’s family needs to know how she got sick – and how so many other members of their family also were exposed to Burkholderia psuedomallei. How can they prevent continuing exposure if they don’t know the source of the bacteria?
“Our first thing is we don’t want anyone to be sick or have a chance of getting sick down the road,” Kennon, who is serving as a spokesperson for the family, told me. “Ultimately no one wants to go through the same thing that Lylah’s gone through.”
CDC: Bacteria strain in outbreak not previously reported by scientists
The family has answered investigators’ questions and provided samples of their blood and a wide range of household products, many of them liquid, plus plants and garden soil that the little girl might have been exposed to. Kennon said the CDC has told the family the preliminary tests on all of their products have been negative for bacteria.
Investigators from the CDC and state health departments are grappling with a limited and challenging set of clues spread across multiple states, Bower said in an emailed response to my questions.
First, there are only three cases in the entire United States that have been identified in this outbreak. And their illnesses developed at different times: The adult who died was sickened in March. Lylah and the other adult who was hospitalized were sickened in May.
The investigation has found few things in common among the three cases, Bower said. And because infections from Burkholderia pseudomallei can develop days, months or sometimes even years after exposure, it is difficult for investigators to even determine when the patients were exposed to the bacterium. And there is the potential of many exposure incidents because of the delayed onset of symptoms.

Bower and CDC officials would not discuss any of the outbreak cases, nor would they say how many family members of the cases in Kansas and Minnesota have received positive antibody tests for exposure to Burkholderia pseudomallei.
“In general, the presence of antibodies means a person may have been exposed to the bacterium, but it does not mean that they will get sick,” Bower said. “The vast majority of melioidosis cases occur within 21 days post exposure, with a few documented cases developing months or years later.” In most cases, the person’s body fights off the bacteria and they will never become ill, he said.
Bower said that, in general, treatment is not recommended based only on a single antibody test, without additional testing or the presence of symptoms.
Melioidosis infections can be treated with certain kinds of antibiotics.
The CDC said the genomic sequence of the bacteria strain involved in the outbreak has never previously been deposited in public databases used by scientists studying a wide range of pathogens and how they evolve. The agency did not answer questions about what country the strain is most closely associated with. It has said only that it is not a strain found in people who have been sickened in the Americas.
For Lylah, 'it's progress every day'
Since the CDC started informing Lylah’s family members of their antibody tests late Friday, they have been trying to figure out why some tested positive for exposure and some did not, even in the same households.
For example, Lylah’s parents, Josy and Dustin, were negative for any antibodies. But Lylah’s 1-year-old sister, Addie, tested positive.
“It’s just crazy to me that you have two little girls who are positive for it but their parents aren’t,” Kennon said.

Kennon tested positive, as did her 7-year-old son. But her 5-year-old son, who spent far more time with Lylah, tested negative.
That kind of pattern played out throughout the family’s households, Kennon said. Seven tested positive, six tested negative. The CDC tested only members of the family who had close contact with Lylah, so not everyone was tested, she said.
Although he is not involved in the CDC investigation, Alfredo Torres, who has studied Burkholderia pseudomallei as a researcher at the University of Texas Medical Branch in Galveston, said this hit-and-miss pattern makes him suspect the source is possibly something they have eaten.
One common way people become infected is by having a cut come into contact with contaminated soil or water.
“It’s very unlikely that the two kids have lesions in their skin, the same with the aunt and the cousin,” Torres, a professor of microbiology and immunology, told me.
These bacteria can infect through the intestinal tract, and it’s possible that not everyone who consumed the same product would have necessarily had an exposure and developed antibodies, he said. The amount of bacteria may have varied in individuals’ portions, or different people could have eaten different amounts.
“This is unfortunately something that was imported by some company, but we don’t know exactly what it is,” said Torres.
It’s discouraging to Lylah’s family to hear that the source of their exposures might be impossible to find.
“One of the things we’re always left with is the why: Why did this happen?” said Kennon. “It’s just scary not knowing.”
But the family is grateful. “Lylah is here, and we know one (of the outbreak cases) didn’t make it,” Kennon said.
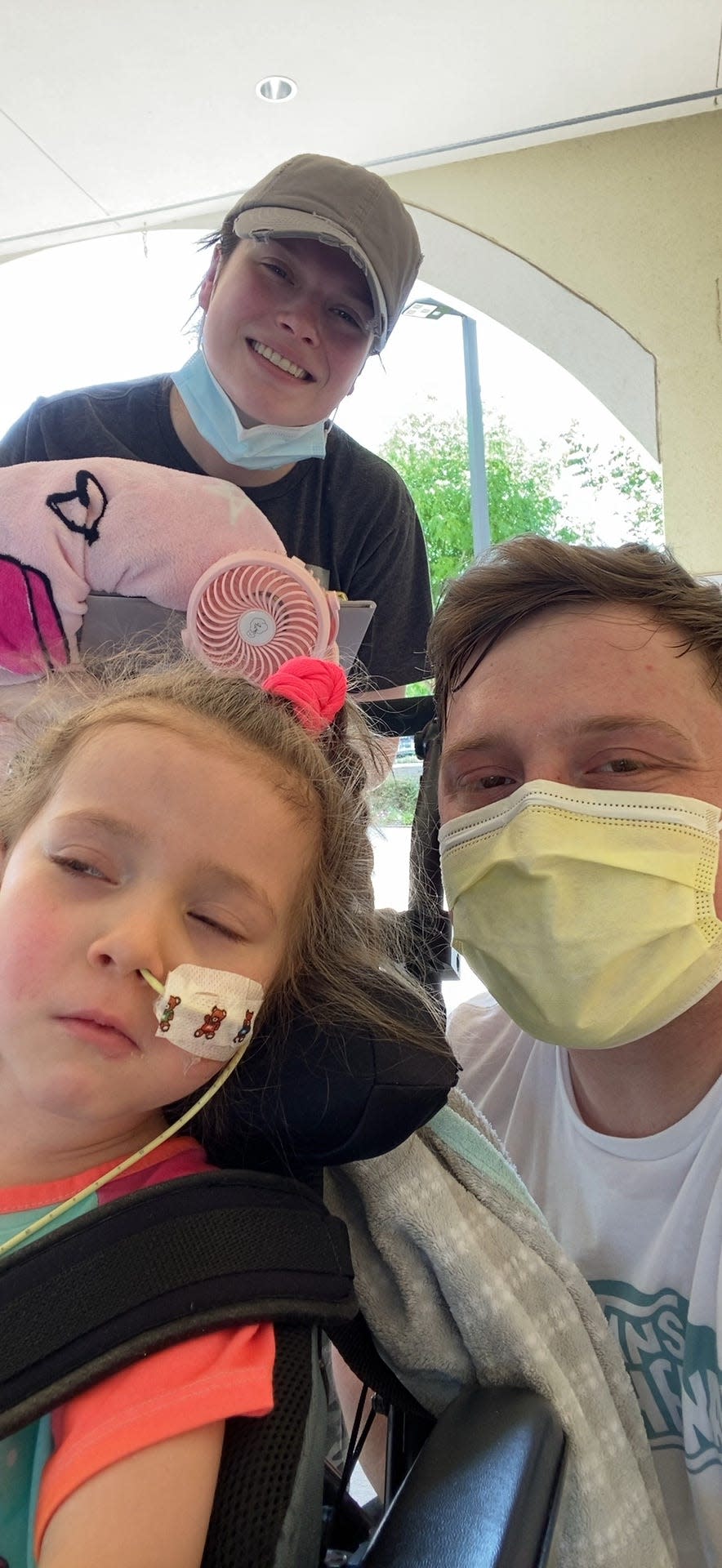
Lylah was transferred recently from Children’s Medical Center Dallas to nearby Our Children’s House, a rehabilitation hospital, where she is receiving intensive speech, physical and occupational therapy.
“Lylah is doing a little bit better. She actually got to go outside Saturday for a little bit for the first time,” Kennon said. Because she cannot swallow, she will receive a permanent feeding tube in a few weeks, allowing the removal of her nasal tube.
“It’s progress every day,” said her aunt. She’s able to move her arms against gravity, and she has been able to make more distinguishable sounds. Her family is preparing to bring her home in mid-August.
Kennon said the generosity of USA TODAY readers has helped the family replace a compact car with a small SUV that will be able to accommodate Lylah’s wheelchair to what will be many trips for physical therapy. After the July 11 article about Lylah’s illness, the family’s GoFundMe page grew from about $6,000 to more than $41,000.
For now, the family is still hoping that investigators are able to find answers – so that nobody else is sickened like Lylah.
Alison Young is an investigative reporter in Washington, D.C. She is also the Curtis B. Hurley Chair in Public Affairs Reporting at the Missouri School of Journalism. During 2009-19, she was a reporter and member of USA TODAY’s national investigative team. Follow her on Twitter: @alisonannyoung
You can read diverse opinions from our Board of Contributors and other writers on the Opinion front page, on Twitter @usatodayopinion and in our daily Opinion newsletter. To respond to a column, submit a comment to letters@usatoday.com.
This article originally appeared on USA TODAY: CDC: Source of foreign bacteria that sickened Texas girl a mystery

 Yahoo Movies
Yahoo Movies 
