NHS ‘bursting at the seams’ as waiting list hits record high
The NHS is “bursting at the seams” as waiting lists hit a record high, while A&E departments experienced their worst performance on record, according to new data.
Figures from NHS England show 7.2 million people were waiting to start routine treatment at the end of October, up from 7.1 million in September and the highest number since records began in August 2007.
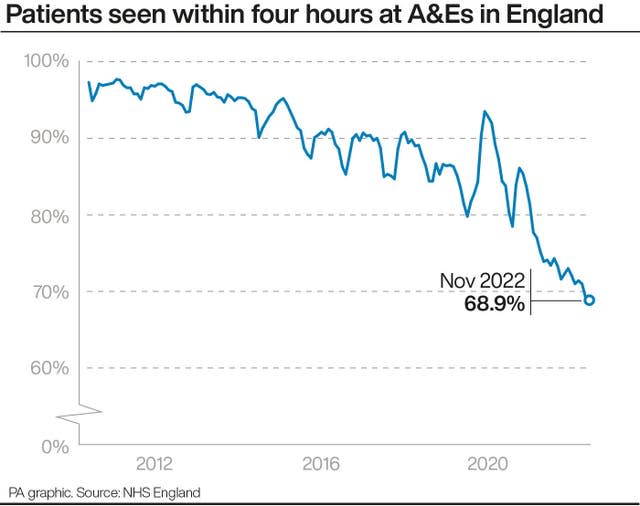
Meanwhile, in emergency departments, just 68.9% of patients in England were seen within four hours last month, down from 69.3% in October and the worst performance on record.

The target is for at least 95% of patients attending A&E to be admitted, transferred or discharged within four hours, but this has not been met nationally since 2015.
Danielle Jefferies, from the King’s Fund, said: “The latest figures show an NHS bursting at the seams as services head into winter struggling to meet sharply rising demand while keeping patients safe.”
The figures do show some improvements to NHS performance in several areas, with the number of people waiting more than 12 hours in A&E departments from a decision to admit to actually being admitted showing a fall.
Some 37,837 people waited longer than 12 hours in November, down 14% from the record 43,792 in October, but still the second-highest monthly total in data going back to August 2010.
The number waiting at least four hours from the decision to admit to admission also dropped from a record 150,922 in October to 143,949 in November.
Regarding the waiting list for planned treatment, such as hip and knee replacements or cataract surgery, some 1,907 people in England were waiting more than two years at the end of October, down slightly from 2,239 at the end of September and well below the peak of 23,778 in January.
However, an estimated 410,983 people in England had been waiting more than 52 weeks, up from 404,851 at the end of September, and equivalent of around one in 18 people on the entire waiting list.
There were some improvements on cancer, although there was a decline on the 62-day (two month) target for starting a first treatment.
Only 60.3% of the 14,425 cancer patients urgently referred by their GP had waited less than than two months by the time they started treatment – the second-lowest percentage on record and below the 85% target.
Elsewhere, 239,180 urgent cancer referrals were made by GPs in England in October, the highest number for that month in records going back to 2009.
This is down from 251,977 referrals in September, but the sixth highest number of monthly referrals on record.
Meanwhile, the proportion of cancer patients in England who saw a specialist within two weeks of being referred urgently by their GP increased from a record low of 72.6% in September to 77.8% in October, but still below the 93% target.

On ambulances, the average response time in November for ambulances in England outside London dealing with the most urgent incidents was nine minutes and 26 seconds, down from nine minutes and 56 seconds in October.
The target is seven minutes. Data for London is not available.
Ms Jefferies, from the King’s Fund, said: “Improving ambulance delays has been a Government priority for some time, but today’s numbers show that one in seven ambulances are delayed by more than an hour as they wait for stretched A&E teams to assess patients.
“Even after a patient’s condition has been deemed serious enough to warrant admission, 38,000 patients are stuck in A&E for over 12 hours because hospitals are too full to admit them.
“Problems at the hospital front door are indicative of issues at the back door.
“The number of patients stuck in hospital despite being well enough for discharge remains alarmingly high at 13,300 – 30% higher than this time last year.
“People are being stranded in hospital because of a long-term lack of investment in social care and NHS community services.

“It is easy to become numb to dire NHS performance figures, but the health service really is facing the toughest pressures since modern records began.
“Industrial action is imminent, more than 50,000 NHS staff are off due to illness, cold weather is biting, and Covid-19, Strep A and other winter viruses will likely increase demand for services.
“All combined, this puts immense strain on staff in health and care services who are having to go above and beyond to support patients.
“Sadly, there are no immediate solutions or quick fixes; these are widespread issues that will require actions across the whole health and care system and it will take time for any improvements to be felt by patients.”
NHS England said tens of thousands more people got the diagnostic tests and checks they needed in October with over 63,000 more compared to the previous month (just over 2m in October, up from 1.99m in September).
The NHS also saw its highest number of ambulance callouts for serious illness for any November on record, while A&E dealt with more attendances than any previous November.
National clinical director for urgent and emergency care, Professor Julian Redhead, said: “Despite the ongoing pressures on services which are exacerbated by flu hospitalisations, issues in social care meaning we cannot discharge patients who are ready, and record numbers needing A&E, staff have powered through to bring down some of our longest waits for care.
“We have already said we are dealing with a perfect storm of pressures this winter, including increased demand for emergency are, and today announced an expansion of mental health crisis services which will ensure people suffering a mental health crisis get the help they need as quickly as possible, and reduce the chances of a patient needing to go to A&E.
“That is all on top of the measures announced NHS’ winter plan published in October which includes new hubs dedicated to respiratory infections and a falls response service to free up ambulance capacity.”

 Yahoo Movies
Yahoo Movies 
