Hyperbaric oxygen therapy is touted as treatment for brain injury, but questions remain
Each year, millions of Americans sustain a traumatic brain injury.
An estimated 11% to 23% of the troops deployed to Iraq and Afghanistan incurred what has been called the wars’ “signature injury” and linked to alarming rates of suicide.
Even mild brain injuries can lead to cognitive impairments, mood changes and other symptoms that can last for months or longer, but there are few effective treatments.
“Despite recent progress in understanding what happens in the brain following TBI, more than 30 large clinical trials have failed to identify specific treatments that make a dependable and measurable difference in people with TBI,” the National Institute of Neurological Disorders and Stroke said in a 2020 report, using the shorthand for the injuries.
One of the interventions tested in those trials, hyperbaric oxygen therapy, is nonetheless advertised as a scientifically proven treatment.
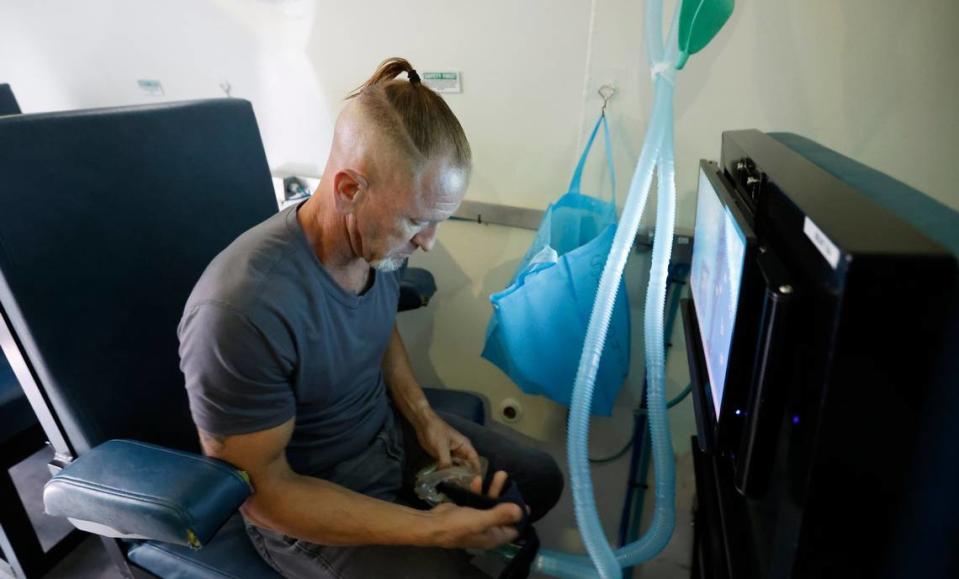
Edward di Girolamo, the owner of a wellness clinic in Research Triangle Park and host of a YouTube show about hyperbaric oxygen therapy, calls it an “established solution” for mild traumatic brain injuries, the type incurred by most people, including soldiers.
He and other boosters have sought to have politicians override the scientific establishment’s reluctance to endorse widespread use and commit government funds to pay for it.
At the state level, they have had success. North Carolina’s General Assembly passed a bill in 2019 authorizing hyperbaric oxygen therapy as a treatment for traumatic brain injuries and post-traumatic stress disorder and later allocated $250,000 to a program targeted at military veterans.
WHAT IS HYPERBARIC OXYGEN THERAPY?
Hyperbaric oxygen therapy, called HBOT for short, involves breathing pure oxygen in a chamber with above-normal air pressure. The additional pressure helps flood the patient’s blood and tissues with oxygen, which can lead to other physiological changes.
The Food and Drug Administration has cleared hyperbaric chambers for treating 13 conditions, including radiation injuries, carbon monoxide poisoning and decompression sickness.
Research has shown that increasing oxygen in the blood has widespread effects, including inhibiting inflammation and mobilizing stem cells.
These effects inspire hope that the therapy can be more broadly applied.
Complications are relatively rare, mainly involving injuries to the middle ear.
But HBOT is resource intensive. A common course of treatment involves 40 sessions in a chamber with each session lasting more than an hour.
WHAT’S THE EVIDENCE?
Advocates who argue that HBOT is an effective treatment for mild traumatic brain injuries often point to personal testimony and studies involving a small number of research participants as proof of effectiveness.
Some preliminary studies describing the experience of a small group of patients reflected improvements in post-concussion symptoms, cerebral blood flow and quality of life.
But both individual stories and case series aren’t considered conclusive evidence of widespread promise. It’s not clear whether the examples described are typical or extraordinary.
“The thing that tends to happen a lot of times is, somebody will treat with hyperbaric oxygen a few dozen people, and one or two of them have a dramatic improvements, and those individuals — common or uncommon in the group — will get touted as this is what happens, you know, we can bring people back to life,” said Dr. Richard Moon, director of Duke University’s respected hyperbaric center.
“But you don’t really know how many there are. Was it one out of 50? Or one out of 100? Or is it 90% of them?”
Scientists find more persuasive proof in randomized controlled trials, which include large numbers of research participants and methods to guard against the placebo effect and other variables that might muddy investigators’ conclusions.

For a treatment to be endorsed as effective by the Food and Drug Administration and the Undersea and Hyperbaric Medical Society, the preeminent physicians’ group in the field, the results must be corroborated by other researchers as well.
So far, that hasn’t happened.
Questions about how to control for the placebo effect in these studies remain under intense debate.
The Veterans Health Administration, in a 2021 report reviewing the evidence, concluded that researchers had not convincingly established that HBOT led to either short-term or long-term improvements in post-concussion and PTSD symptoms among people who sustained a mild traumatic brain injury.
Then last year, spurred by promising research out of Israel, a committee of the Undersea and Hyperbaric Medical Society debated whether to recommend adding mild traumatic brain injury as an approved use of HBOT. But they too concluded there’s still not enough proof.
The determination could change as additional research is published, said Moon, an anesthesiologist and pulmonary medicine specialist who is a member of that committee. At least one randomized controlled trial is currently recruiting.
Moon rejects the argument made by boosters like di Girolamo that mainstream scientists are ignoring solid proof to protect their financial self-interest, the government’s or the pharmaceutical industry’s.
“If hyperbaric oxygen dramatically improved people’s brains and IQ after head injury, why wouldn’t we want to do it?” he said. “I mean, we would all want to help people.”
WHAT ABOUT ‘MILD’ HYPERBARIC OXYGEN THERAPY?
With celebrity endorsements from the likes of LeBron James and Justin Bieber, soft-sided hyperbaric chambers have been gaining popularity in recent years.

They are not interchangeable with traditional, hard-walled hyperbaric chambers, and there’s much less evidence to support their use.
The FDA endorses the soft-sided devices, which look like human-sized zippered bags, only for treating altitude sickness.
But wellness companies, including Restore Hyper Wellness, a franchise business expanding rapidly in the Triangle, tout the devices as effective for many other conditions, including traumatic brain injuries.
The advertising for “mild” hyperbaric oxygen therapy is frequently misleading, the Undersea and Hyperbaric Medical Society says, because the soft-walled chambers cannot reach pressures high enough to be therapeutic.
The American Medical Association adopted a resolution last year that opposed mild hyperbaric oxygen therapy “unless and until effective treatments can be delivered safely in facilities with appropriately trained staff including physician supervision and prescription and only when the intervention has scientific support or rationale.”
The devices, particularly when paired with an oxygen concentrator, pose fire and suffocation risks, according to the UHMS, fire officials and the FDA.
Last year, several North Carolina cities ordered businesses to stop using soft-walled chambers, saying they did not meet safety standards.
Journalist Carli Brosseau is a former investigative reporter at The News & Observer.

 Yahoo Movies
Yahoo Movies 
