Growing fears as doctors face prioritising some patients over others
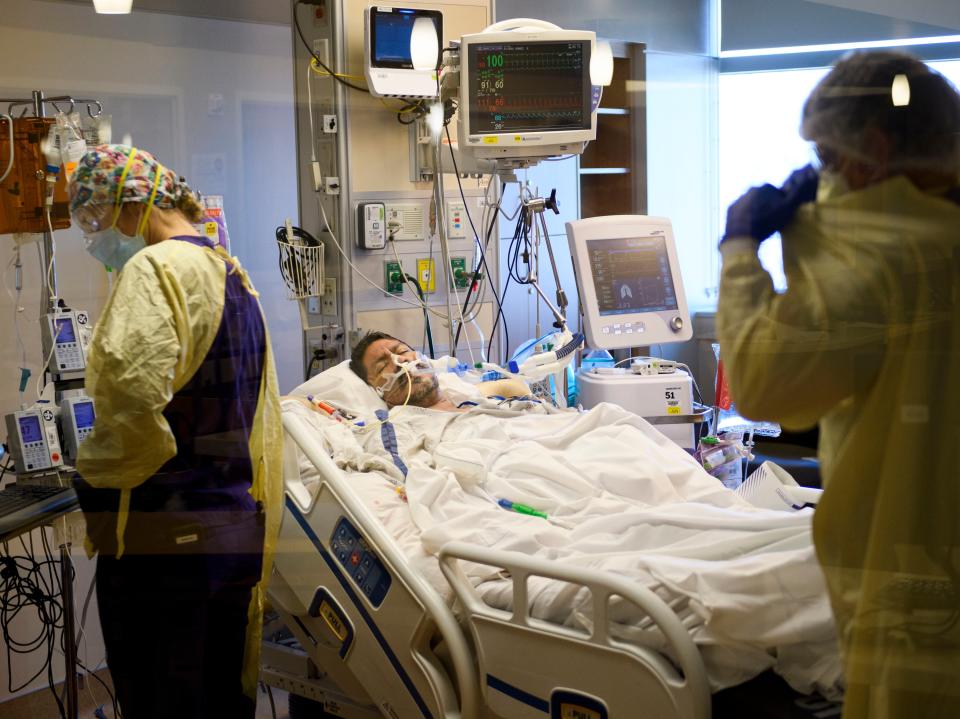
Intensive care units across the NHS are already overwhelmed by Covid patients
(AFP via Getty)Doctors across the NHS face an “immediate reality” of having to choose which patients are prioritised for care as the numbers of coronavirus cases continue to surge across the country.
At one hospital trust, medics have been told they may have to accept a “just good enough” standard of care for patients in coming weeks, while the medical regulator has said it recognised difficult decisions were being made “day after day, shift after shift” across the country.
The situation facing many hospitals has prompted renewed calls for national advice to clinicians on how they should approach the so-called rationing of care – where treatment choices are balanced against the resources available and the needs of other patients.
The Nuffield Council on Bioethics has said doctors must be given clear guidance about how to handle such situations while the president of the Intensive Care Society warned the NHS faces the “greatest risk” since the start of the pandemic that such decisions may have to be made.
Ethics committees, made up of senior clinicians, have been established by most hospitals offering advice to the front line over decisions including whether patients should be admitted to intensive care. Doctors are also sharing amongst themselves their own frameworks for decision-making, such as a special Covid mortality calculator.
Many hospitals across the southeast, London, midlands and east of England regions have seen ICU bed occupancies of 150 per cent or higher. Many NHS trusts have been forced to open makeshift ICUs in operating theatres and general wards to cope with the increased demand.
In a letter to doctors at East Suffolk and North Essex NHS Trust on Tuesday, chief executive Nick Hulme said he accepted doctors were feeling “vulnerable both personally and professionally” as they were redeployed to different areas to cope with the surge in Covid patients.
He said: “With the significant pressure of caring for so many more sick patients in our hospitals, necessary changes in admission and discharge thresholds and also the impact on patients waiting for outpatient care or procedures, we may not be able to provide care to our patients to the level we would all wish.
“We may have to accept a standard that is ‘good enough’ to bring benefit to the greatest number of patients who require our care.”
One doctor at the trust told The Independent: “We are all getting annoyed with the read in-between the lines and keep it politically correct messaging. For transparency the messaging should be clear: ‘patient care will suffer and everyone will have to accept it’. That is where we are or will be if things carry on like this.
“It’s not a position any of us in the profession want to be in.”
The General Medical Council (GMC) has issued ethical advice to doctors about the decisions they face when a hospital is overwhelmed. The GMC chair, Dame Clare Marx, told medics this week that the regulator would consider the context doctors were working in when judging their actions if complaints were made about them later.
A coalition of health bodies has written to health secretary Matt Hancock, urging the government to update the law to ensure medical workers do not feel “vulnerable to the risk of prosecution for unlawful killing” when treating coronavirus patients “in circumstances beyond their control”.
The letter, coordinated by the Medical Protection Society (MPS), and signed by the British Medical Association, Doctors’ Association UK, the Hospital Consultants and Specialists Association, the Royal College of Surgeons of Edinburgh, the British Association of Physicians of Indian Origin and Medical Defence Shield, said emergency legislation is needed to protect doctors and nurses from “inappropriate” legal action over Covid-19 treatment decisions.
The health groups argued that there is no legal protection for Covid-related issues such as when there are “surges in demand for resources that temporarily exceed supply”.
The health groups wrote: “With the chief medical officers now determining that there is a material risk of the NHS being overwhelmed within weeks, our members are worried that not only do they face being put in this position but also that they could subsequently be vulnerable to a criminal investigation by the police.”
Dave Archard, chair of the Nuffield Council on Bioethics, said fears over the first wave led to discussions over national guidance for treatment decisions during the pandemic, but they never came to fruition.
In a statement he added: “Nearly one year on, record increases in daily Covid-19 cases combined with routine winter pressures in the NHS threaten to overwhelm and engulf. These decisions are no longer a worst-case scenario, but an immediate reality.
“In the event that demand outstrips supply, how should clinical teams proceed? Should they prioritise the worst-off patients most in need of treatment? Or should they choose those with the greatest chance of survival? Is it simply chance of survival that is relevant or is a matter of considering quality of life in that survival? Can it be justified to prioritise younger patients over older patients? Is that discriminatory?
“These are not just matters of intellectual curiosity, but are the questions needing answered on the front line.”
He called on the government to issue national guidance to doctors to help them decide how patients should be prioritised adding leaving it to local hospitals was “manifestly unjust.”
“It is unfair to the clinicians working under extreme pressure, under fear of litigation or professional sanction, and at risk of severe moral distress,” he said.
There are concerns over the longer-term effects of such guidance on treatment decisions in intensive care and so far neither the government or the NHS has been willing to officially offer a formal view.
Some clinicians fear the consequences of setting down in policy the route by which doctors could be allowed to choose between patients, which would include denying admission to ICU but also turning off a patient’s ventilator in favour of another patient. But others argue it would be better to have a standard agreed by which decisions could be measured.
One central London doctor told The Independent these decisions were being taken already.
They said: “We’re close to the situation where we won’t have ICU beds for patients we can actually save. We need to be very selective on who we admit. The frail over-70s with previous comorbidities are so sick they’re just not surviving.”
Stephen Webb, president of the Intensive Care Society, told The Independent: “There still remains a risk we will get to a stage where intensive care units are overwhelmed. We are not at that stage yet, but that is only because of the efforts staff are putting in to make sure that doesn’t happen.
“But we are at the greatest risk of this happening so far in the pandemic. We have more patients than in wave one and fewer staff to look after them. There is a risk of care quality diminishing.
“The ICS absolutely understands the call for guidance on prioritisation of patients for ICU admission. We welcome the statement from the Nuffield Council on Bioethics which shed light on this controversial issue. None of us ever want to be in the position of making decisions to choose between patients because of limited resources.
“Developing such guidance will be tremendously difficult and complex. As doctors we are used to making difficult decisions about individual patients but choosing between patients because of lack of staff or resources is a new paradigm.
“We should not get to the position of having to make these decisions until the whole country is saturated and every ICU is full. Until then the ICS believes normal clinical decision-making should continue to apply.”
Intensive care doctor Rupert Pearse, who works at the Royal London Hospital, said: “The burden of decision-making around ICU admission traditionally falls on senior ICU doctors. Most of us are privately very worried about what will happen if we run out of resources. The false suggestion that we rationed ICU beds in the first wave has upset a lot of people.
“I am not aware of any patient who was not admitted to intensive care during the pandemic when the ICU consultants responsible believed that they should be. But we would be failing in our duty if we do not plan for this situation.”
He said a new level of alert for critical care units, or critcon levels, were valuable in showing the pressure on services but he added: “Our decisions remain subjective, individual and personal. We are lacking guidance from society.”
In a message to doctors on Monday, Dame Clare Marx, chair of The General Medical Council, said: “As doctors, we have always made difficult decisions under pressure. Covid presents many with even greater challenges. The escalating pandemic means some of you are having to make such judgements, day after day, shift after shift. This unrelenting pressure can exact a heavy toll.
“I know how anxious some doctors are about the way in which actions and decisions taken in this environment may be reviewed. I want to reassure you that, should any concern be raised, the context in which a doctor is working will be fully taken into account.”
The government’s Moral and Ethical Advisory Group was asked to draw up a policy on Covid-19 triage last year which included scoring patients to decide whether they would, for example, receive intensive care, but it was never formally released.
A draft was later published by the Intensive Care Society but with the scoring and triage thresholds removed.
In a statement, Nick Hulme, chief executive of East Suffolk and North Essex Foundation Trust, said: “The increase in patients with Covid-19 in our hospitals means that we are having to provide care differently, and we sent a letter to thank our clinical staff for their flexibility. We are still providing safe and effective care to all of our patients and no care is being rationed in any way.”
The Department of Health and Social Care was asked if it had a response to the call for national guidance but declined to respond.
NHS England also declined to offer a substantive comment on the issue but instead said NHS staff had worked hard to create extra capacity and urged the public to follow the rules to prevent hospital admissions.

 Yahoo Movies
Yahoo Movies 