Covid-19 infections falling, but picture uncertain in some English regions
The number of people with Covid-19 in homes across England continues to fall, though the picture is uncertain in some regions, new data shows.
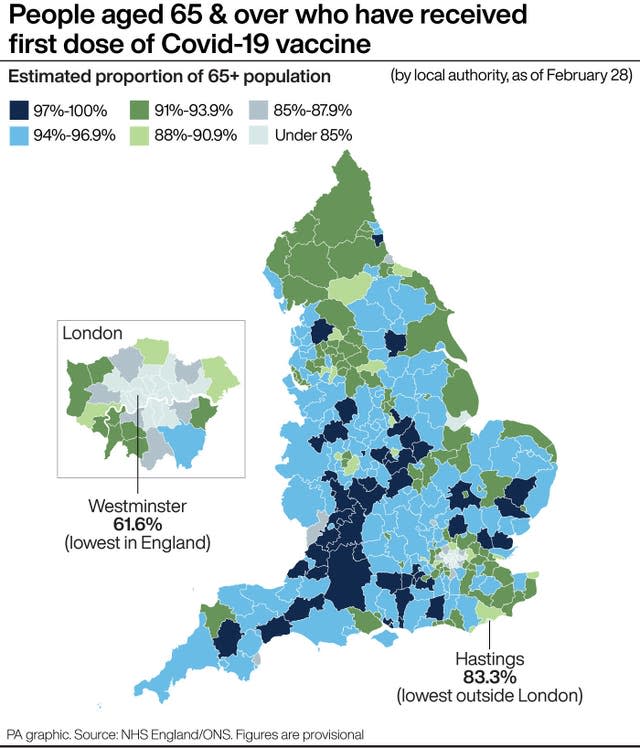
Figures from the Office for National Statistics (ONS) estimate that around one in 220 people in private households in England had Covid-19 between February 21 and 27 – the equivalent of 248,100 people.
The figure is down from around one in 145, or 373,700 people, for the period February 13 to 19, and is the lowest figure since the week to October 1 when it was one in 240.
However, the number of people infected in England is still high when compared to last summer. In the week to August 25 around one in 2,000 people had coronavirus.
The ONS said the percentage of people testing positive for Covid-19 in the latest figures had decreased in all regions except for north-east England, the East Midlands and eastern England, where it said the trend was uncertain.
North-east England had the highest proportion of people of any region in England likely to test positive for coronavirus in the week to February 27 – around one in 150 people.
The West Midlands had the next highest estimate at one in 160, while the figure was one in 185 for the East Midlands; one in 190 for north-west England; one in 195 for London; one in 225 for Yorkshire and the Humber; one in 260 for eastern England; one in 340 for south-east England, and one in 365 for south-west England.
In Wales, the latest estimate was one in 285, down from 205, and in Northern Ireland it was one in 325, down from one in 195.
The estimate for Scotland for the week to February 27 was around one in 335 people, down from one in 225.
The latest data is based on swab tests from 684,875 people in the UK, regardless of whether they had symptoms, and does not include hospitals and care homes.
We are offering households, and support and childcare bubbles, of school and college aged children regular #COVID19 testing.
Find out more 👇
— Department of Health and Social Care (@DHSCgovuk) March 5, 2021
It comes as Government scientific advisers said the latest reproduction number (the R) estimate for England remains unchanged at between 0.7 and 0.9.
Meanwhile, R is between 0.7 and 0.9 for the whole of the UK, compared with 0.6 and 0.9 last week.
Estimates of R are below 1 in all NHS regions of England, although the estimate for the North East and Yorkshire has an upper bound of 1.
The Scientific Pandemic Influenza Group on Modelling (SPI-M) said: “Although the epidemic continues to decrease nationally, there may be more variation in transmission locally, with some indications that the rate of decline in infections could be slowing in some areas.”
Earlier, one adviser said society will need to learn to live with a “substantial” degree of Covid-19 mortality.
Professor Andrew Hayward, from the Scientific Advisory Group for Emergencies (Sage), said the number of deaths will continue to drop as vaccination kicks in, and death rates could begin to look more like those for flu.
Other experts, including Professor Paul Hunter, from the University of East Anglia, have said the UK can expect a wave of deaths next winter, mostly among the unvaccinated and those for whom vaccines do not provide total protection.
Prof Hayward told Times Radio: “I think given the societal trade-offs, we are going to have to live with a degree of mortality that will be substantial.
“I think it will get less over time as more people get vaccinated, and as more people get immune, and I do believe that we’ve been through the worst of this.”
Prof Hayward said he does not think new variants of Covid-19 will completely evade the protection offered by vaccines.
A study this week found that between 25% and 61% of people in the Brazilian city of Manaus were susceptible to reinfection with the worrying P1 strain, which has also been found in six people in the UK.
Vaccine manufacturers are working on updated vaccines to tackle variants, which could be fast-tracked for approval by the autumn.
Prof Hayward said: “The vaccines will still take the sting out of it, if you like, and reduce the case fatality rates.
“Of course we have the technology to update the vaccines and I think that’s where we’re going really, a situation that will be much more like flu. The numbers of deaths will be much more like flu, the approach to surveillance of new strains and development of new vaccines and regular annual vaccinations will be like that.
“And we will get back to normal.”
Asked if he thought epidemiologists did not really have the ear of Government in early March last year, before the first lockdown, Prof Hayward said: “I think there was conflicting advice… there was some advice if you go too early then people will get tired of it, but it did seem to be fairly inevitable that we would need to do something like that at some stage.
“I think the timing of it was something that they were getting conflicting advice on.
“However, I think we didn’t learn our lesson from that and we didn’t really learn the lesson that lockdowns are going to be way, way more effective if you start them earlier.”
Prof Hayward said it was much easier to put out a very small fire than a big forest blaze.
“When it came to the following autumn, we didn’t learn that lesson,” he said.
Looking back at the beginning of the pandemic, he added: “I think one of the reasons that we’ve had so many deaths is that we left things far too late in terms of taking more restrictive measures.
“By the time you start to see major increases in deaths then it was really too late to take action, and hence the levels got extraordinarily high before we took effective action, and it took a long, long time for them to go back down again.”

 Yahoo Movies
Yahoo Movies 
