Confusion and fear as Australia’s aged care workers wait to be vaccinated with winter looming
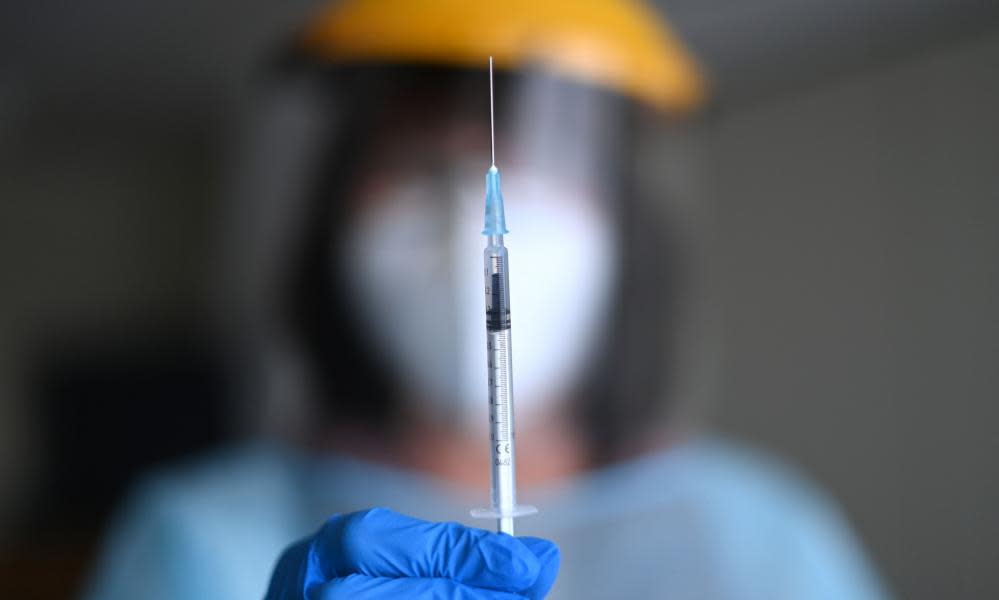
The aged care sector has warned the government to drastically improve its vaccine rollout to aged care staff before winter, saying it is vital that workers be “given priority and vaccinated quickly”.
Advocates have also warned that people with a disability, including group home residents and those in regional areas, are still missing out on their Covid-19 vaccinations.
The health department announced on Thursday that almost 2.9m Australians have been vaccinated, including about 279,986 in aged and disability care.
Related: Young Australians with disabilities lose out as Pfizer vaccine is rolled out to under-50s
But the department’s daily data releases do not give specific figures on the vaccination of either the aged care workforce or those in disability care, two areas where the rollout is lagging badly.
Both cohorts were included in the highest-priority group – phase 1a – but the rollout plan has since shifted repeatedly.
Initially, aged care workers were to receive their jab from an in-reach team, which visited their facility separately to aged care residents. The in-reach teams, in many cases, did not show up, and staff were left in limbo.
As recently as last month, the federal government still did not have a clear plan for vaccinating aged care workers under the age of 50.
Now they are being told to get their vaccine either from a GP, state-run hubs, the commonwealth-run respiratory clinics, or wait for an in-reach team to show up.
Leading Age Services Australia, a peak group for aged care, has warned the government the rollout has been too slow for critical aged care staff.
Chief executive Sean Rooney said his organisation has been “disappointed with the timeliness and comprehensiveness of the responses to the issues raised by the Department of Health”.
“We welcome the extended rollout since the beginning of May, especially for residents,” he said in a statement to the Guardian. “But it is vital that the aged care workforce is given priority and vaccinated quickly, particularly as we head into winter.
“We are still seeing periodic outbreaks across the nation and we must prioritise vaccinations to save older people and the staff who look after them.”
The aged care services minister, Richard Colbeck, told the ABC on Thursday morning that the government was “80% of the way through the sector” for vaccination of aged care residents.
“We’ll have all aged care residents having had their first dose in the next couple of weeks, so that process has settled really well,” he said.
Related: What is the Moderna vaccine? And will it boost Australia’s Covid vaccination program?
The government wanted to get the workforce vaccinated “as soon as possible”, Colbeck said. But the minister said the plans had to change due to the new advice on AstraZeneca.
“Because of the health advice that we’ve received with respect to AstraZeneca, we’ve had to reset the workforce rollout. So we now have a number of different pathways for the aged care workforce to access the vaccine, that’s through state clinics, it’s through their GPs, it’s through some in-reach into residential aged care facilities.”
The Australian Nursing & Midwifery Federation, which represents aged care nurses, said the change in plans had contributed to significant confusion for workers.
ANMF federal secretary Annie Butler said the rollout had improved since the state-run vaccine hubs had begun vaccinating aged care workers.
But she said the changing plans had created confusion among staff.
“It’s still confused because they’ve now got so many different things in the mix of where they can get it,” Butler told the Guardian.
“We do think that some of the issues have settled a little because the state vaccination centres have opened up to aged care workers, and so that has helped to make it easier. There is just confusion, though, about the dedicated pop-up hubs which are just for aged care and disability care workers.”
The federal government is also not providing daily updates on its vaccine rollout in disability care. Last month, though, health officials told a Senate committee hearing that fewer than 7% of disability care residents had received a single dose of vaccine.
Earlier this week, it was revealed that prioritising the Pfizer vaccine for residents under 50 had caused havoc with the rollout to young people in group homes, due to the logistical barriers in storing and delivering the vaccine.
The federal health department acknowledged it was yet to finalise a new plan to vaccinate younger Australians in disability care, and was still negotiating with states and territories.
Advocacy group People with Disability Australia (PWDA) on Thursday wrote to all state and territory disability ministers to urge for improvements in the rollout.
PWDA president Samantha Connor said people with a disability and their support workers were still experiencing difficulties in access, particularly in Western Australia, where people with Down’s syndrome were reportedly unable to access the Pfizer vaccine.
It also reported variable access for people living in regional and remote settings, congregate settings, and for young people in higher-risk categories.
PWDA warned there was a lack of available information on potential AstraZeneca side-effects for older people with a disability.
“People in group homes, and rural and remote areas are missing out on vaccines across the nation,” Connor said.
“We need to make sure people at risk of adverse outcomes from Covid-19 can be vaccinated, including our clinically vulnerable people younger than 50.”

 Yahoo Movies
Yahoo Movies 
